Introduction
Chronic pancreatitis is a medical condition characterized by long-term inflammation of the pancreas. This condition can lead to various complications, including bile reflux. In this article, we will explore the causes, symptoms, and treatment options for chronic pancreatitis and bile reflux.
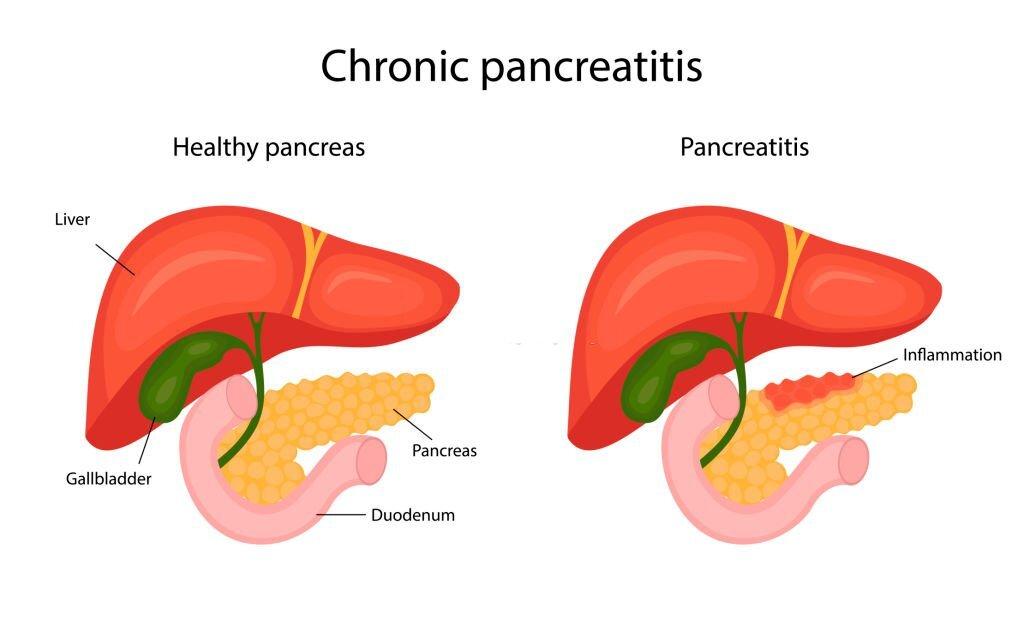
Understanding Chronic Pancreatitis
Chronic pancreatitis refers to the persistent inflammation of the pancreas, a vital organ located in the abdominal region. The pancreas plays a crucial role in the digestion and regulation of blood sugar levels. When the pancreas becomes inflamed, it can lead to various complications.
Causes of Chronic Pancreatitis
Several factors can contribute to the development of chronic pancreatitis. The most common cause is prolonged alcohol abuse, which damages the pancreatic tissues over time. Other causes include gallstones, certain genetic conditions, and autoimmune diseases.
Symptoms of Chronic Pancreatitis
The symptoms of chronic pancreatitis can vary from person to person. Common signs and symptoms include persistent abdominal pain, weight loss, oily and foul-smelling stools, nausea, and vomiting. In advanced stages, individuals may also experience diabetes due to impaired insulin production.
Introduction to Bile Reflux
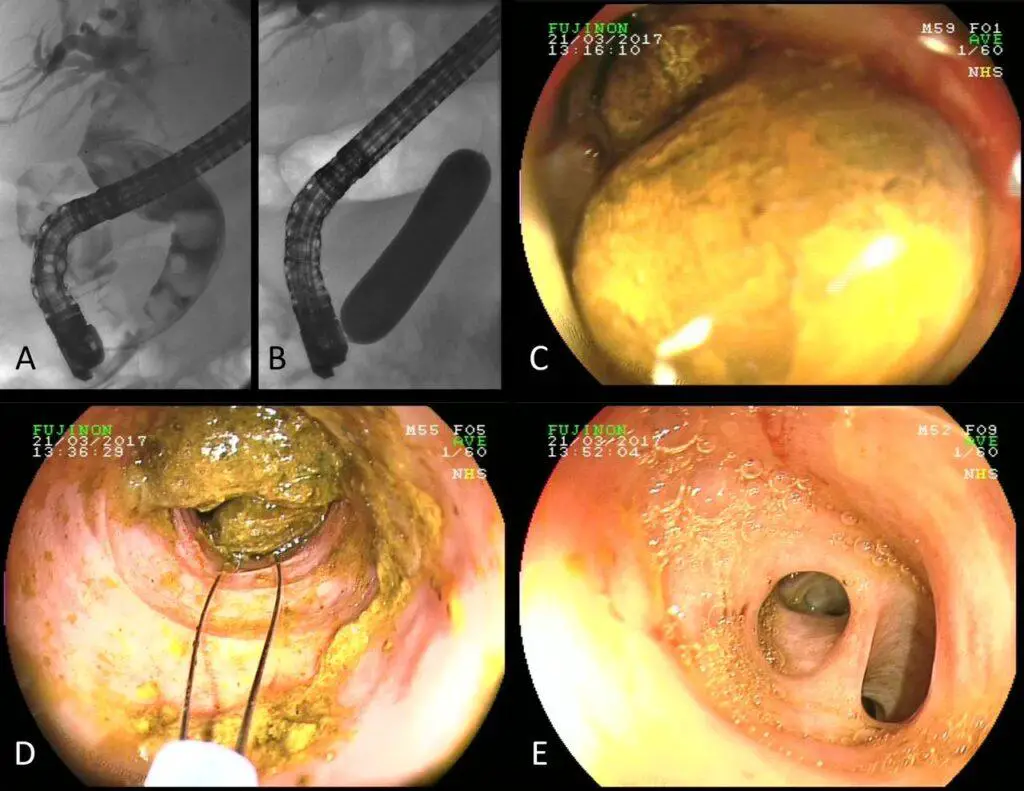
Bile reflux occurs when bile, a digestive fluid produced in the liver, flows back into the stomach and even reaches the esophagus. Usually, the pyloric valve, located at the junction between the stomach and small intestine, prevents the backflow of bile. However, in certain cases, this valve may malfunction, leading to bile reflux.
Bile reflux is not a new condition. The surgeons have frequently found bile in the stomach during surgery, for over a hundred years. The presence of bile is a regular finding by gastroscopy in persons with stomach inflammation-gastritis, ulcers, after gallbladder surgery, and gastroesophageal reflux disease (GERD). In 70% of the chronic cases of heartburn and Barrett’s Esophagus, there is bile reflux. Barrett’s Esophagus is a serious precancerous complication of GERD.
The Link between Chronic Pancreatitis and Bile Reflux
Chronic pancreatitis can cause structural changes in the pancreas and disrupt the normal flow of digestive enzymes. These changes can impair the function of the pyloric valve, increasing the risk of bile reflux. The presence of bile in the stomach and esophagus can further aggravate the symptoms of chronic pancreatitis.
Nowadays, there are more evidence that bile reflux in combination with acid reflux leads to serious injury of the stomach and esophagus. This injury does not fall from the sky; therefore, as same as in the case of chronic pancreatitis, bile reflux has also three stages: functional, structural, and final. You understand that by reading Three Stages of Chronic Pancreatitis.
- Acidic pancreas and bile– fictional stage
- Pancreatic deficiency-structural stage
- Pancreatic failure
What can cause bile reflux in a person with the different stages of chronic pancreatitis?
Under normal circumstances, the liver produces alkaline bile, while the pancreas manufactures highly alkaline pancreatic juice enriched with digestive enzymes. The alkaline nature of these fluids promotes healthy digestion and ensures their proper flow.
Conversely, when acidic changes occur, they disrupt digestion and lead to an inappropriate reverse flow. In the illustration, it is evident that in the case of bile reflux, the aggressive mixture of bile and pancreatic juice is regurgitated into the stomach, causing inflammation likened to a burning sensation.
Why does it happen? Let us explain.
Bile is an alkaline fluid consisting of a delicate balance of water, bicarbonates, minerals, lecithin, cholesterol, bile pigments, bile acids, and bile salts. If bile becomes acidic, bile acids begin to precipitate. It is widely known that bile acids possess an extraordinary degree of chemical aggressiveness. They render the acidic bile highly corrosive and irritating. Consequently, the acidic bile causes irritation and damage to the surrounding tissues, including bile ducts, the gallbladder, and the sphincter of Oddi. This, in turn, leads to spasms, inflammation, and ulcers. When the aggressive acidic mixture of bile and pancreatic juice reaches the duodenum, it can trigger chaotic spasms, resulting in its regurgitation into the stomach and, in some cases, even the esophagus. This is what we refer to as bile reflux.
In the fictional stage of acidic pancreas and bile, individuals may experience occasional heartburn following a large, fatty meal accompanied by alcohol consumption. Laboratory tests may appear normal, although a gastroscopy might reveal mild inflammation in the duodenum and stomach. Typically, patients are diagnosed with GERD and treated with stomach acid suppressors. Unfortunately, if the person continues to lead an acidic lifestyle and consume alcohol, their condition will progressively worsen.
In the pancreatic deficiency-structural stage, individuals suffer from persistent heartburn, accompanied by possible regurgitation of sour-tasting contents from the stomach into the throat, frequent belching, gas, nausea, vomiting, upper abdominal pain, and other symptoms. Symptomatic therapy may provide temporary relief or prove ineffective. A gastroscopy would reveal severe inflammation, ulcers, and deformation in the duodenum, as well as inflammation, ulcers, and traces of bile in the stomach. Inflammation in the esophagus may also be observed. This stage requires significant lifestyle changes, alterations in dietary habits, correction of the acid-alkaline balance, restoration of beneficial intestinal bacteria, addressing deficiencies of vital nutrients, improving digestion, and implementing a combination of conventional and alternative treatments.
Failure to address these issues can lead to pancreatic failure. In addition to the symptoms associated with chronic pancreatitis, such as constant abdominal and chest pain, indigestion accompanied by chronic diarrhea and oily stool, nausea, vomiting, weight loss, and fatigue, a gastroscopy may reveal the presence of Barrett’s Esophagus.
In the case of chronic pancreatitis and bile reflux, the conventional treatment of heartburn using stomach acid suppressors may not be entirely appropriate. Recent medical research indicates that Proton Pump Inhibitors (PPIs), such as Prilosec (Omeprazole), diminish pancreatic function, resulting in deficiencies of essential vitamins, minerals, and trace elements. Some medical studies even suggest that Prilosec may cause acute pancreatitis. If the proton ion-H+ fails to enter the stomach acid and instead remains in the bloodstream, it could lead to systemic acidity known as metabolic acidosis. Always remember, acidity can harm the pancreas.
It is evident that prioritizing a healthy, slightly alkaline environment throughout the entire body, especially in the liver and pancreas, can reduce the occurrence of bile/pancreatic reflux into the stomach and esophagus. Consequently, this approach can minimize bile reflux and alleviate persistent heartburn in individuals with chronic pancreatitis.
[su_box title=” ” box_color=”#ee6409″] The whole body’s acidity can be managed in a few ways:
To promote a healthy alkaline environment in the body and alleviate the occurrence of bile reflux and persistent heartburn in individuals with chronic pancreatitis, the following measures can be adopted:
- Incorporate alkaline-forming, natural foods into your diet.
- Drink healing mineral water, such as Karlovy Vary, known for its therapeutic properties.
- Consider consuming alkaline mineral supplements like Cellular Magnesium-Potassium.
- Cease the use of toxic acid-forming substances like alcohol or certain medications.
- Take measures to control dysbiosis, such as addressing small intestine bacterial overgrowth (SIBO) and Candida yeast overgrowth.
- Engage in whole body cleansing practices to promote overall wellness.
By following these steps, you can support a balanced acid-alkaline equilibrium in your body, particularly in the liver and pancreas, which can help reduce bile/pancreatic reflux into the stomach and esophagus, thereby minimizing bile reflux and persistent heartburn associated with chronic pancreatitis.
[/su_box]
Although the alkaline diet and mineral supplementation are well-known among individuals with chronic pancreatitis, it is true that Karlovy Vary healing mineral water is relatively new to Americans. Drinking healing mineral water has been a longstanding medical practice in Europe for centuries. Located in the Czech Republic, Karlovy Vary is a renowned health mineral spa situated in the heart of Europe. Millions of individuals experiencing digestive and pancreatic symptoms, including heartburn, stomach fullness, nausea, cramps, chronic abdominal pain, diarrhea, and constipation, have found relief by consuming this healing mineral water. For those unable to visit Karlovy Vary, geyser water has been vaporized to create mineral salt as an alternative.
Most individuals suffering from chronic pancreatitis and bile/pancreatic reflux often experience additional issues such as Candida yeast overgrowth and small intestine bacterial overgrowth (SIBO). These conditions contribute to regular fermentation in the intestines, leading to the production of a significant amount of toxic gases. As these gases are released, they can cause the valve between the esophagus and stomach, known as the lower esophageal sphincter (LES), to open. When this valve opens, the contents of the stomach are forced up into the esophagus, resulting in severe heartburn.
[su_note note_color=”#f1d78f”]
If you suffer from chronic pancreatitis and experience persistent heartburn accompanied by bitter regurgitations, and if medications that suppress stomach acidity fail to provide relief, there is a high possibility that you are dealing with bile reflux. Addressing bile reflux is not a straightforward task, but alternative medicine and a natural approach that focuses on treating the underlying issues can be beneficial. It is crucial to avoid misdiagnosis or merely treating the symptoms of bile reflux, as this may result in serious complications such as inflammation and ulcers in the stomach and duodenum, as well as the development of Barrett’s esophagus and esophageal cancer.
[/su_note]
Prevention Tips
While it may not be possible to prevent all cases of chronic pancreatitis and bile reflux, some preventive measures can reduce the risk. These include practicing moderation in alcohol consumption, maintaining a healthy diet, managing underlying medical conditions, and seeking timely treatment for gallstones or other pancreatic disorders.
Conclusion
Chronic pancreatitis and bile reflux are interconnected conditions that can significantly impact an individual’s quality of life. Recognizing the causes, symptoms, and available treatment options is crucial for effectively managing these conditions. By adopting a multidisciplinary approach that combines medication, lifestyle modifications, and surgical interventions, individuals can find relief and minimize the impact of chronic pancreatitis and bile reflux.
FAQs
- Is chronic pancreatitis curable? Chronic pancreatitis is a chronic condition that cannot be completely cured. However, with appropriate treatment and lifestyle modifications, symptoms can be managed effectively.
- Can chronic pancreatitis lead to pancreatic cancer? Although chronic pancreatitis is a risk factor for pancreatic cancer, the majority of individuals with chronic pancreatitis do not develop cancer. Regular medical follow-ups and early detection can help monitor any potential cancerous changes.