Introduction
Barrett’s esophagus is a condition that affects the lining of the esophagus, the tube that connects the throat to the stomach. It is characterized by changes in the cells lining the lower part of the esophagus, which can increase the risk of developing esophageal cancer. In this article, we will discuss the symptoms, causes, and treatment options for Barrett’s esophagus.
1. Understanding Barrett’s Esophagus
Barrett’s esophagus is a condition where the normal tissue lining the esophagus is replaced by tissue similar to that found in the intestines. This change is often associated with long-term gastroesophageal reflux disease (GERD), a condition in which stomach acid flows back into the esophagus.
Related Article On Gallstones and Bile Duct Stones
2. Symptoms of Barrett’s Esophagus
Most individuals with Barrett’s esophagus do not experience any specific symptoms. However, they may have symptoms related to GERD, such as heartburn, regurgitation, difficulty swallowing, or chest pain.
3. Causes and Risk Factors of Barrett’s Esophagus
The exact cause of Barrett’s esophagus is unknown, but it is believed to be related to long-term exposure to stomach acid. The following factors may increase the risk of developing Barrett’s esophagus:
- Chronic gastroesophageal reflux disease (GERD)
- Obesity
- Smoking
- Age (over 50)
- Male gender
4. Diagnosis and Screening
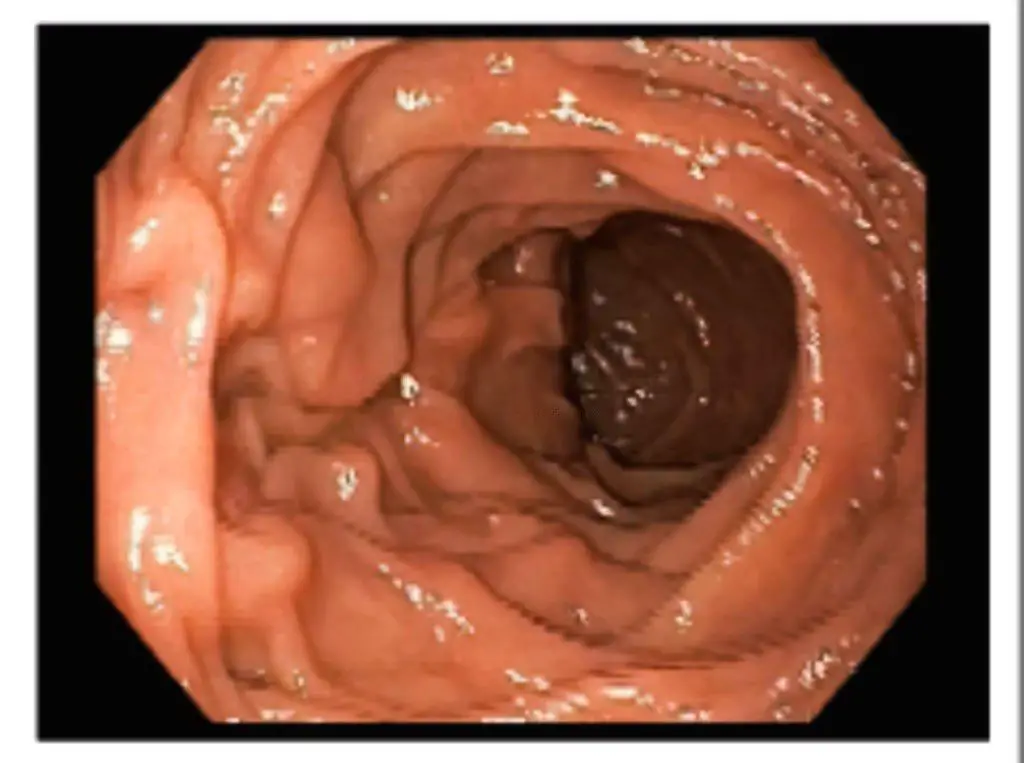
Barrett’s esophagus is diagnosed through an upper endoscopy, where a thin, flexible tube with a camera is inserted into the esophagus to examine the lining. During the procedure, the doctor may take a biopsy of the tissue for further analysis.
5. Treatment Options For Barrett’s Esophagus
The treatment approach for Barrett’s esophagus depends on the presence of abnormal cells and the risk of developing esophageal cancer. The following treatment options are available:
5.1 Lifestyle Modifications
- Weight loss for overweight individuals
- Avoiding foods that trigger acid reflux
- Elevating the head of the bed while sleeping
- Eating smaller, more frequent meals
- Quitting smoking
5.2 Medications
- Proton pump inhibitors (PPIs) to reduce acid production
- H2 blockers to decrease acid production
- Antacids to neutralize stomach acid
5.3 Endoscopic Treatments
- Radiofrequency ablation (RFA) destroys abnormal tissue
- Cryotherapy to freeze and destroy abnormal cells
- Photodynamic therapy (PDT) using laser and light-sensitive drugs
5.4 Surgical Procedures
- Esophagectomy to remove the affected portion of the esophagus
- Endoscopic mucosal resection (EMR) to remove abnormal tissue
6. Follow-Up Care and Monitoring
After treatment, regular follow-up appointments are necessary to monitor the condition and check for any changes. This may include repeat endoscopies and biopsies to evaluate the progression of the disease.
7. Complications and Prevention
Barrett’s esophagus increases the risk of developing esophageal cancer, although the majority of individuals with Barrett’s esophagus do not develop cancer. To reduce the risk, it is important to manage GERD symptoms, undergo regular screenings, and follow the prescribed treatment plan.
8. Diet and Nutrition
Adopting a healthy diet and making certain lifestyle changes can help manage GERD symptoms and reduce the risk of complications. It is advisable to:
- Avoid spicy, fatty, and acidic foods
- Limit alcohol and caffeine consumption
- Eat smaller meals and avoid late-night eating
- Maintain a healthy weight
- Stay hydrated
Frequently Asked Questions (FAQs)
- Can Barrett’s esophagus be cured?
- Barrett’s esophagus cannot be cured, but it can be managed and monitored effectively.
- Is Barrett’s esophagus the same as esophageal cancer?
- Barrett’s esophagus is a condition that can increase the risk of developing esophageal cancer, but not everyone with Barrett’s esophagus develops cancer.
- How often should I undergo screening for Barrett’s esophagus?
- The frequency of screenings depends on individual factors and the presence of abnormal cells. Your doctor will guide the recommended screening intervals.
- Can lifestyle modifications alone treat Barrett’s esophagus?
- Lifestyle modifications can help manage GERD symptoms and reduce the risk of complications, but they may not be sufficient as the sole treatment for Barrett’s esophagus.
- What are the chances of developing esophageal cancer with Barrett’s esophagus?
- The risk of developing esophageal cancer in individuals with Barrett’s esophagus is relatively low, but regular monitoring and appropriate treatment are crucial to minimize the risk further.
Conclusion
Barrett’s esophagus is a condition that requires careful management and monitoring. By understanding the symptoms, causes, and available treatment options, individuals with Barrett’s esophagus can take appropriate steps to minimize the risk of complications and maintain their overall health. If you have persistent GERD symptoms or suspect you may have Barrett’s esophagus, consult with your healthcare provider for proper evaluation and guidance.