Introduction
After undergoing gallbladder surgery, some individuals may experience a condition known as Sphincter of Oddi Dysfunction (SOD). This article aims to provide a comprehensive understanding of SOD, its causes, symptoms, diagnosis, treatment options, and recovery. We will explore the impact of gallbladder surgery on the Sphincter of Oddi and how it can lead to dysfunction. Additionally, we will address frequently asked questions regarding this condition to provide further clarity and insight.
What is the Sphincter of Oddi?
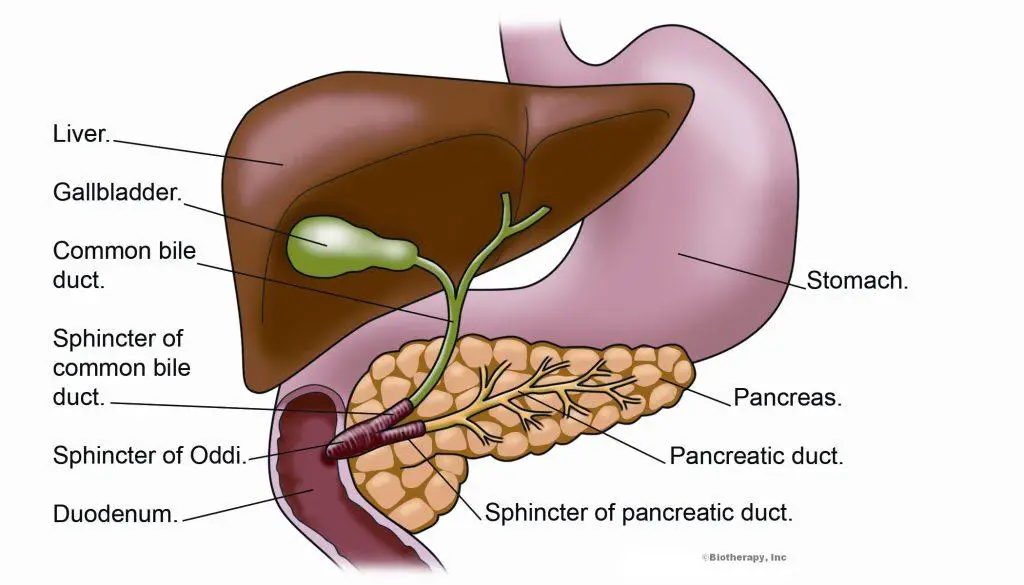
The Sphincter of Oddi is a muscular valve located in the small intestine, specifically at the junction where the bile duct and pancreatic duct meet. Its primary function is to regulate the flow of bile and pancreatic juices into the digestive system, aiding in digestion. The sphincter remains closed most of the time, opening only when food enters the small intestine.
Understanding Gallbladder Surgery
Gallbladder surgery, known as cholecystectomy, is a common procedure performed to remove the gallbladder. This surgery is often recommended when the gallbladder becomes inflamed or when gallstones develop. While the gallbladder’s removal does not typically result in significant digestive problems, in some cases, it can lead to complications such as Sphincter of Oddi Dysfunction.
The liver provides a chemical called bile to the digestive process, and the pancreas provides pancreatic juice. These important chemicals flow from the liver and pancreas into the small intestine to help with digestion. The flow of these chemicals is controlled by a muscle called the sphincter of Oddi.
A sphincter is a muscle (usually round) that can open and close. When it’s working properly, the sphincter of Oddi opens to allow bile and pancreatic juice to flow through and then closes again. However, in a condition called sphincter of Oddi dysfunction, the sphincter muscle does not open when it should. This prevents the bile and pancreatic juice from flowing through and causes a backup of digestive juices. The backup can cause bouts of severe pain in the abdomen.
[su_note note_color=”#f1d78f”]
There are two basic types of sphincter of Oddi dysfunction:
- If the digestive juices are backing up in the bile ducts from the liver, the term is biliary dysfunction.
- If the backup is occurring in the pancreas, you may hear your doctor use the term “pancreatitis.” This means the pancreas is becoming inflamed.
[/su_note]
There are also three categories of sphincter of Oddi dysfunction:
[su_list icon=”icon: star” icon_color=”#172a85″]
- In categories I and II, doctors can find clear evidence of the dysfunction, such as abnormal blood test results or a dilated bile duct, which might be found by using an ultrasound test.
- In category III dysfunction, there are no clear-cut lab findings or abnormalities, and the only evidence of the dysfunction is abdominal pain. The pain is believed to be caused by a sudden spasm of the sphincter of Oddi. Type III dysfunction is much more difficult for doctors to diagnose.
[/su_list]
[su_box title=” ” box_color=”#ee6409″]
Symptoms of Sphincter of Oddi Dysfunction
Individuals with SOD may experience a range of symptoms, including:
- Abdominal pain, often in the upper right quadrant
- Nausea and vomiting
- Bloating and indigestion
- Jaundice (yellowing of the skin and eyes)
- Back pain
- Diarrhea or changes in bowel movements
These symptoms can vary in intensity and duration, with some individuals experiencing mild discomfort while others may have more severe and prolonged symptoms.
What are the symptoms of sphincter of Oddi dysfunction?
Abdominal pain is the most common symptom; less common symptoms include nausea, vomiting, fever, chills, and diarrhea. These symptoms can come and go and can be mild one time and severe the next.
How is the sphincter of Oddi dysfunction diagnosed?
When a sphincter of Oddi dysfunction is suspected, your doctor will first check to see if the abdominal pain is caused by another condition. It is important to make sure patients with abdominal pain don’t have serious conditions such as cancer of the pancreas or bile ducts, peptic ulcer disease, or stones in the ducts that carry the bile from the liver. In some cases, even heart conditions such as angina or ischemia can cause pain that seems to be coming from the abdomen.
Your doctor may want to take a close look at the sphincter of Oddi to see if it is functioning normally. This is done by placing a small plastic tube into the pancreas duct or bile duct near the sphincter of Oddi to measure how well it is contracting and expanding. Patients are placed under sedation for this procedure, which is called sphincter of Oddi manometry.
[/su_box]
[su_note note_color=”#f1d78f”]
Treatment Options for Sphincter of Oddi Dysfunction
The treatment approach for SOD aims to relieve symptoms and improve the patient’s quality of life. Depending on the severity of the condition, several treatment options may be considered, including:
Medications for Symptom Relief
Certain medications, such as antispasmodics and analgesics, can be prescribed to manage abdominal pain and reduce sphincter spasms. These medications work by relaxing the sphincter and relieving discomfort.
Endoscopic Interventions
Endoscopic procedures, such as sphincterotomy, can be performed to widen the sphincter and improve the flow of bile and pancreatic juices. This procedure involves making a small incision in the sphincter to alleviate its tightness and promote better drainage.
Surgical Approaches
In severe cases where other treatments have been ineffective, surgical interventions may be considered. Surgical options include sphincteroplasty, which involves repairing the sphincter, or sphincter resection, which involves removing the sphincter altogether. These procedures aim to restore normal sphincter function and alleviate symptoms.
Dietary and Lifestyle Modifications
Making certain dietary and lifestyle modifications can also help manage SOD symptoms. It is recommended to follow a low-fat diet, avoid trigger foods, maintain a healthy weight, and engage in regular physical activity. These lifestyle changes can promote better digestion and reduce the risk of symptoms.
Recovery and Post-Surgery Care
After undergoing treatment for Sphincter of Oddi Dysfunction, it is important to follow the recommended post-surgery care instructions. This may include taking prescribed medications, adhering to dietary guidelines, attending follow-up appointments, and gradually resuming normal activities. The recovery period can vary depending on the chosen treatment approach and the individual’s overall health.
Conclusion
Sphincter of Oddi Dysfunction can be a challenging condition to manage, particularly for individuals who have undergone gallbladder surgery. Understanding the causes, symptoms, diagnosis, and treatment options is crucial for effectively addressing this condition. By working closely with healthcare professionals and making necessary lifestyle modifications, individuals with SOD can find relief and improve their quality of life.
FAQs (Frequently Asked Questions)
- Is Sphincter of Oddi Dysfunction a common complication after gallbladder surgery? Sphincter of Oddi Dysfunction is not a common complication after gallbladder surgery, but it can occur in some individuals.
- Can the Sphincter of Oddi Dysfunction resolve on its own without treatment? In some cases, mild forms of Sphincter of Oddi Dysfunction may resolve on their own without specific treatment. However, it is important to consult with a healthcare professional for proper evaluation and guidance.
- Are there any long-term complications associated with Sphincter of Oddi Dysfunction? If left untreated, Sphincter of Oddi Dysfunction can lead to recurrent pain, inflammation, and complications such as pancreatitis and cholangitis.
References
- International Foundation for FuThe Cleveland Clinic Foundationnctional Gastrointestinal Disorders. Sphincter of Oddi Dysfunction Accessed 9/17/2013.
- Hogan WJ. Gastroenterol Hepatol (N Y). 2007;3(1):31-5. Diagnosis and treatment of sphincter of oddi dysfunctionAccessed 9/17/2013
- Marks JOddionsky JL. Chapter 3. In: Zinner MJ, Ashley SW, eds. Maingot’s Abdominal Operations. 12th ed. New York: McGraw-Hill; 2013. Endoscopy and Endoscopic Intervention Accessed 9/17/2013
[/su_note]