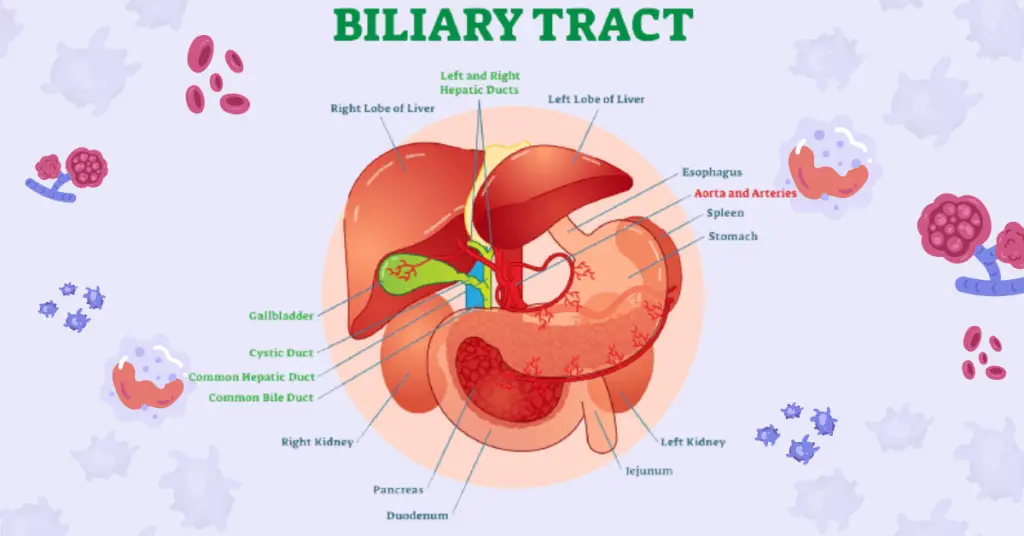
The gallbladder is a small, pear-shaped organ located beneath the liver. Its primary function is to store bile, a digestive fluid produced by the liver. Cholecystectomy is the surgical procedure performed to remove the gallbladder. In this article, we will explore the reasons for cholecystectomy, the different types of procedures, the recovery process, and the potential risks and benefits associated with gallbladder removal.
Introduction: Understanding Cholecystectomy
Cholecystectomy is the surgical removal of the gallbladder. It is often recommended when the gallbladder becomes inflamed, infected, or contains gallstones. Gallstones are hardened deposits that form inside the gallbladder and can cause severe pain and other complications. Cholecystectomy is a common procedure and is usually performed using minimally invasive techniques
[su_note note_color=”#f1d78f”]
Types of cholecystectomies:
The gallbladder may be removed in one of two ways: [su_list icon=” icon: star” icon_color=”#172a85″]
- Open Cholecystectomy: In some cases, open cholecystectomy may be necessary. This procedure requires a larger incision in the abdomen to access and remove the gallbladder. Open cholecystectomy is typically performed when laparoscopic techniques cannot be used due to factors such as severe inflammation, scarring, or other complications.
- Laparoscopic Cholecystectomy: Laparoscopic cholecystectomy is the most common method of gallbladder removal. It involves making several small incisions in the abdomen, through which a laparoscope (a thin tube with a camera) and surgical instruments are inserted. The surgeon uses these instruments to visualize and remove the gallbladder. Laparoscopic cholecystectomy is preferred due to its minimally invasive nature, shorter recovery time, and reduced risk of complications.
[/su_list] [/su_note]
A laparoscopic cholecystectomy is considered a minimally invasive procedure that typically has a shorter recovery time compared to open cholecystectomy. However, there may be cases where the gallbladder appears severely diseased during a laparoscopic examination or other complications arise, requiring the surgeon to perform an open surgical procedure to safely remove the gallbladder.
Purpose of the Procedure
A cholecystectomy may be performed for various reasons, such as the presence of gallstones (cholelithiasis), inflammation or infection of the gallbladder (cholecystitis), or the presence of gallbladder cancer. Gallbladder inflammation or infection can cause pain, which may be described as follows:
[su_list icon=”icon: star” icon_color=”#172a85″]
is typically located on the right side of the upper abdomen may be constant or intensify after a heavy meal sometimes feels more like fullness rather than pain can be felt in the back and the tip of the right shoulder blade
[/su_list]
Additional symptoms of gallbladder inflammation or infection include, but are not limited to, nausea, vomiting, fever, and chills. It’s important to note that symptoms of gallbladder problems can resemble other medical conditions or issues, and each individual may experience symptoms differently. Consulting a physician is always recommended for an accurate diagnosis. Your physician may have other reasons for recommending a cholecystectomy.
Procedure Risks
Like any surgical procedure, cholecystectomy carries potential complications. Some possible complications include, but are not limited to, the following:
[su_list icon=”icon: star” icon_color=”#172a85″]
- bleeding
- infection
- injury to the bile duct – the tube that transports bile from the gallbladder to the small intestine
- During laparoscopic cholecystectomy, the insertion of instruments into the abdomen can cause injury to the intestines or blood vessels. If you suspect you might be pregnant, it is important to notify your physician. Specific risks may depend on your individual medical condition. It’s essential to discuss any concerns with your physician prior to the procedure.
[/su_list]
Preparation for the Procedure
[su_list icon=”icon: star” icon_color=”#172a85″]
- Your physician will explain the procedure to you and give you an opportunity to ask any questions you may have.
- You will be required to sign a consent form that grants permission for the procedure.
- Carefully read the form and seek clarification if needed.
- In addition to a detailed medical history, your physician may conduct a physical examination to ensure your overall health before the procedure. You may also undergo blood tests or other diagnostic assessments.
- You will be asked to refrain from eating or drinking for eight hours prior to the procedure, usually after midnight.
- If you are pregnant or suspect you might be pregnant, inform your physician.
- Notify your physician of any sensitivities or allergies you have to medications, latex, tape, anesthetic agents (local and general), and any medications (prescribed or over-the-counter) or herbal supplements you are taking.
- Inform your physician if you have a history of bleeding disorders or if you are taking anticoagulant (blood-thinning) medications, aspirin, or other medications that affect blood clotting. It may be necessary to discontinue these medications before the procedure. If the procedure is performed on an outpatient basis, you will need someone to drive you home due to the sedation given during the procedure.
- The surgical site area may need to be shaved. Based on your medical condition, your physician may request additional specific preparations.
[/su_list]
During the Procedure
A cholecystectomy can be performed as an outpatient procedure or as part of a hospital stay. The specific procedures may vary depending on your condition and your physician’s practices. Typically, a cholecystectomy is performed under general anesthesia, while you are asleep.
The general process of a cholecystectomy is as follows:
[su_list icon=”icon: star” icon_color=”#172a85″]
- You will be asked to remove any jewelry or objects that might interfere with the procedure.
- You will be instructed to remove clothing and given a gown to wear.
- An intravenous (IV) line will be inserted into your arm or hand.
- You will be positioned on the operating table lying on your back.
- The anesthesiologist will continuously monitor your heart rate, blood pressure, breathing, and blood oxygen level throughout the surgery
- The surgical site will be cleansed with an antiseptic solution.
[su_box title=” ” box_color=”#ee6409″]
open method cholecystectomy:
- An incision (open method) will be made, either slanting under the ribs on the right side of the abdomen or as a vertical incision in the upper part of the abdomen.
- The gallbladder will be removed.
- In certain cases, one or more drains may be inserted through the incision to allow drainage of fluids or pus.
laparoscopic method cholecystectomy:
- Three to four small incisions will be made in the abdomen. Carbon dioxide gas will be introduced into the abdomen to inflate the abdominal cavity, facilitating better visualization of the gallbladder and surrounding organs.
- A laparoscope will be inserted through one of the incisions, and instruments will be inserted through the other incisions to remove the gallbladder.
- Once the procedure is complete, the laparoscope will be removed.
- completion of both methods: The removed gallbladder will be sent to the laboratory for examination. The skin incision(s) will be closed with stitches or surgical staples. A sterile bandage/dressing or adhesive strips will be applied
[/su_box]
[su_heading size=”20″]After the Procedure[/su_heading]
In the Hospital:
After the procedure, you will be taken to the recovery room for observation. The duration of your recovery process will depend on the type of procedure performed and the anesthesia administered. Once your blood pressure, pulse, and breathing are stable, and you are alert, you will be transferred to your hospital room. If a laparoscopic cholecystectomy is performed on an outpatient basis, you may be discharged from the recovery room to return home.
You may receive pain medication as needed, either administered by a nurse or through a self-administration device connected to your intravenous line. A thin plastic tube may be inserted through your nose into your stomach to remove swallowed air. The tube will be removed once your bowels return to normal function. You will not be able to eat or drink until the tube is removed.
If an open procedure was performed, you may have one or more drains in the incision. The drains will typically be removed within a day or so. It’s possible that you may be discharged with the drain still in place, covered with a dressing. Follow your physician’s instructions for caring for the drain. You will be encouraged to get out of bed within a few hours after a laparoscopic procedure or by the next day after an open procedure.
Depending on your situation, you may be allowed to drink liquids a few hours after surgery. Your diet may gradually progress to more solid foods as tolerated. A follow-up visit with your physician will be scheduled, usually two to three weeks after the procedure.
[su_note note_color=”#f1d78f”]
Conclusion
Cholecystectomy is a common surgical procedure performed to remove the gallbladder. It is recommended for various reasons, such as gallstones, inflammation, and other gallbladder conditions. The surgery can be performed using minimally invasive techniques, allowing for a faster recovery and reduced risk of complications. While there are risks associated with the procedure, the benefits of cholecystectomy often outweigh the potential drawbacks, leading to improved digestive health and relief from gallbladder-related symptoms.
FAQs
1. How long does it take to recover from cholecystectomy?
Recovery time varies, but most individuals can resume normal activities within a week or two after the surgery.
2. Will I have to change my diet after gallbladder removal?
You may need to make dietary adjustments, especially during the initial stages of recovery. Your doctor will provide specific guidelines based on your condition.
Online Resources
The content provided here is for informational purposes only and was not designed to diagnose or treat a health problem or disease or replace the professional medical advice you receive from your physician. Please consult your physician with any questions or concerns you may have regarding your condition.
This page contains links to other Web sites with information about this procedure and related health conditions. We hope you find these sites helpful, but please remember we do not control or endorse the information presented on these Web sites, nor do these sites endorse the information contained here