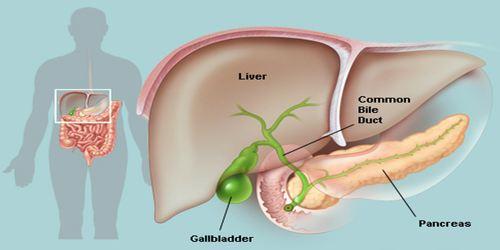
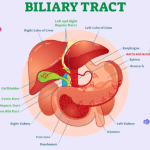
The gallbladder is a small, pear-shaped organ located beneath the liver. Although often overlooked, it plays a crucial role in the digestive system and overall health. In this article, we will explore the importance of the gallbladder and its functions in maintaining our well-being.
1. Introduction
The gallbladder, a small but essential organ, plays a vital role in the digestive process. It aids in the breakdown and absorption of dietary fats, ensuring our bodies can utilize them efficiently. Additionally, the gallbladder can sometimes develop issues, such as the formation of gallstones, which can lead to significant discomfort and require medical intervention.
2. Anatomy of the Gallbladder
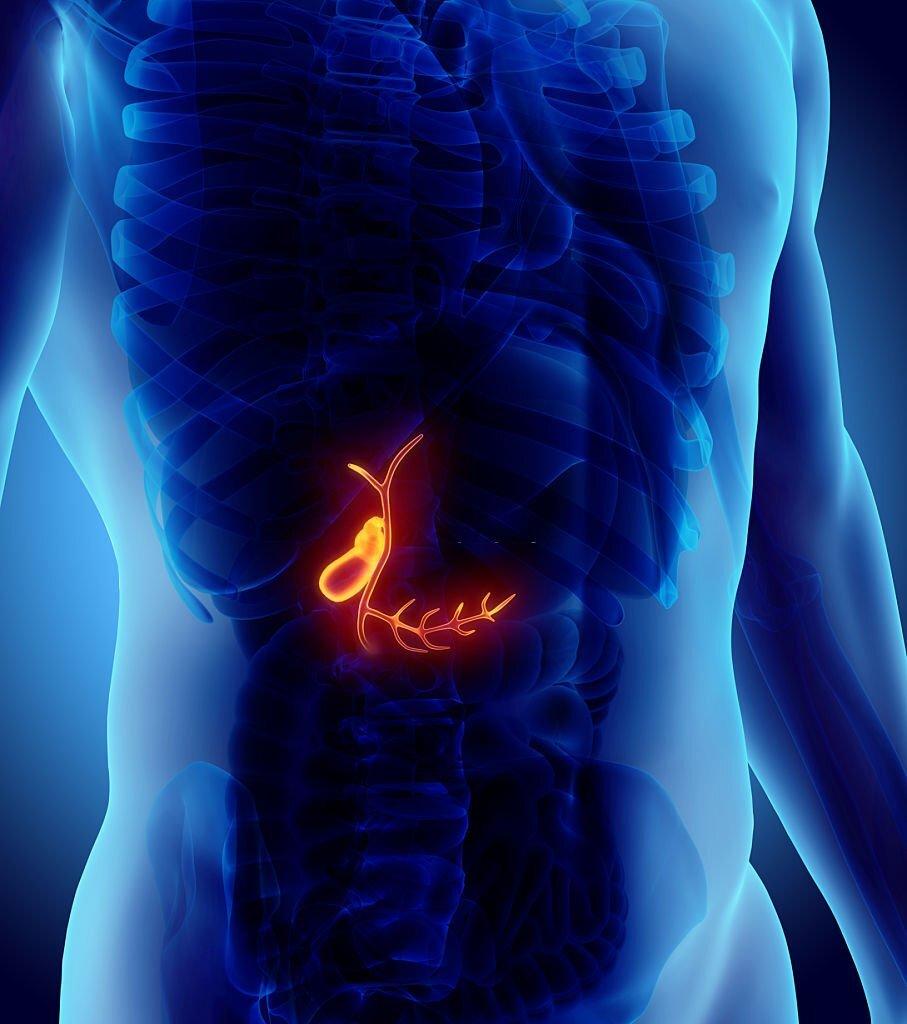
The gallbladder is positioned in the upper right abdomen, nestled beneath the liver. It resembles a small sac and can hold approximately 50 milliliters of bile, a substance produced by the liver. The gallbladder is connected to the liver through a series of ducts, including the common bile duct, which carries bile to the small intestine.
3. Production and Storage of Bile
The liver produces bile continuously, regardless of whether we consume food or not. This yellowish-green fluid is rich in bile salts, cholesterol, water, and waste products. Once produced, bile travels through a network of small ducts until it reaches the common hepatic duct, which connects to the gallbladder. The gallbladder acts as a reservoir for bile, allowing it to concentrate and store until needed.
4. Release of Bile
When we consume a meal, especially one high in fat, our body signals the gallbladder to release bile. This process is triggered by the hormone cholecystokinin (CCK), which is released by the small intestine in response to the presence of fatty foods. Upon receiving the signal, the gallbladder contracts, forcing stored bile back into the common bile duct and eventually into the small intestine.
5. Gallbladder Role in Fat Digestion
The primary function of bile is to aid in the digestion and absorption of dietary fats. Bile salts present in bile break down large fat molecules into smaller droplets through a process called emulsification. This action increases the surface area of fats, allowing enzymes called lipases to efficiently break them down into fatty acids and glycerol. These breakdown products are then absorbed by the small intestine and utilized by the body for energy production and other essential functions.
6. Gallstones and their Impact
Gallstones are solid deposits that form in the gallbladder. They can range in size from tiny particles to larger stones. Gallstones can cause significant discomfort and lead to various complications, such as inflammation of the gallbladder (cholecystitis), bile duct obstruction, or pancreatitis. Factors contributing to gallstone formation include an imbalance in bile composition, obesity, a sedentary lifestyle, and certain medical conditions.
7. Gallbladder Disease
Gallbladder disease refers to any condition that affects the gallbladder’s normal functioning. It encompasses various issues, including gallstones, inflammation, infection, and tumors. Common symptoms of gallbladder disease include abdominal pain, nausea, vomiting, bloating, and indigestion. If left untreated, gallbladder disease can lead to severe complications and impact overall health.
8. Lifestyle Tips for a Healthy Gallbladder
Maintaining a healthy gallbladder is crucial for optimal digestion and overall well-being. Here are some lifestyle tips that can promote gallbladder health:
- Maintain a healthy weight: Obesity increases the risk of gallstone formation. Engaging in regular physical activity and following a balanced diet can help maintain a healthy weight.
- Eat a high-fiber diet: Consuming foods rich in fiber, such as fruits, vegetables, and whole grains, can promote regular bowel movements and prevent gallstone formation.
- Stay hydrated: Drinking an adequate amount of water daily helps maintain the proper concentration of bile in the gallbladder.
- Limit fat intake: While fats are essential for our body, excessive consumption can overload the gallbladder. Opt for healthy fats like those found in avocados, nuts, and seeds.
- Avoid crash diets: Rapid weight loss can increase the risk of gallstone formation. Aim for steady and sustainable weight loss instead.
- Limit alcohol consumption: Excessive alcohol intake can contribute to gallbladder problems. Drink alcohol in moderation or avoid it altogether.
9. Dietary Recommendations
Adopting a gallbladder-friendly diet can help prevent gallstone formation and maintain optimal gallbladder health. Consider incorporating the following dietary recommendations:
- Consume a diet rich in fruits, vegetables, and whole grains.
- Choose lean sources of protein, such as poultry, fish, and legumes.
- Opt for healthy fats, including those found in olive oil, avocado, and fatty fish.
- Limit saturated and trans fats, commonly found in fried foods, processed snacks, and fatty meats.
- Avoid or limit the consumption of high-cholesterol foods, such as organ meats, shellfish, and full-fat dairy products.
- Stay hydrated by drinking an adequate amount of water throughout the day.
- Include foods with natural bile-promoting properties, such as artichokes, turmeric, and dandelion greens.
10. Common Symptoms of Gallbladder Problems
Identifying the symptoms of gallbladder problems is essential for timely diagnosis and treatment. Some common signs include:
- Abdominal pain, particularly in the upper right quadrant or in the middle of the abdomen.
- Nausea and vomiting.
- Bloating and indigestion.
- Belching or gas.
- Changes in bowel movements, such as diarrhea or pale-colored stools.
- Jaundice (yellowing of the skin and eyes).
11. Diagnosing Gallbladder Issues
If gallbladder problems are suspected, a healthcare professional may perform various diagnostic tests, including:
- Ultrasound: This non-invasive imaging technique uses sound waves to create images of the gallbladder and detect abnormalities.
- Blood tests: Blood samples can be analyzed to check for signs of infection, inflammation, or liver function abnormalities.
- Endoscopic retrograde cholangiopancreatography (ERCP): This procedure involves the insertion of a flexible tube with a camera into the digestive tract to examine the gallbladder and surrounding structures.
- Magnetic resonance cholangiopancreatography (MRCP): MRCP uses magnetic resonance imaging (MRI) to obtain detailed images of the gallbladder and bile ducts.
12. Treatment Options
The treatment approach for gallbladder problems depends on the specific condition and its severity. Treatment options may include:
- Medications: Certain medications, such as ursodeoxycholic acid, may help dissolve gallstones or reduce symptoms associated with gallbladder disease.
- Lifestyle changes: Adopting a healthy lifestyle, including maintaining a balanced diet and regular exercise, can improve gallbladder health.
- Surgical intervention: In cases of severe gallbladder disease or recurrent gallstones, surgical removal of the gallbladder (cholecystectomy) may be necessary.
13. Surgical Removal of the Gallbladder
Cholecystectomy is a common surgical procedure performed to remove the gallbladder. It can be done using traditional open surgery or minimally invasive techniques, such as laparoscopic or robotic-assisted surgery. Removal of the gallbladder does not significantly affect digestion, as the bile produced by the liver can still reach the small intestine through an alternative pathway.
14. Post-Gallbladder Removal
After the gallbladder removal, some individuals may experience changes in digestion, particularly when consuming fatty foods. This can lead to symptoms such as loose stools or increased frequency of bowel movements. Adjusting the diet to include smaller, more frequent meals and gradually reintroducing fats can help manage these symptoms. Most individuals adapt well to the absence of a gallbladder over time.
15. Conclusion
The gallbladder plays a crucial role in our digestive system and overall health. It functions to store and release bile, which aids in the digestion and absorption of dietary fats. Maintaining a healthy gallbladder through proper diet, regular exercise, and weight management is essential for preventing gallstone formation and promoting optimal digestive function.
FAQs
1. Can I live a normal life without a gallbladder?
Yes, you can live a normal life without a gallbladder. The liver continues to produce bile, which can reach the small intestine through an alternative pathway after gallbladder removal.
2. Are there any long-term dietary restrictions after gallbladder removal?
Most individuals can resume a normal diet after gallbladder removal. However, some people may need to adjust their fat intake to manage digestion, especially in the initial period after surgery.